Throughout the second half of May I ran my Cystic Fibrosis Around the World blog series. My goal behind the project was to compare the “patient” experience among people living with CF across the globe and learn about the different types of care offered.
It was really a culmination of many weeks of interviews and annoying emails (on my behalf). So I want to start out by saying thank you to all of those involved! To that end, I was humbled to receive so many emails from people all over the world asking to take part in the project. The series will continue sometime in July with interviews from people living with CF in Turkey, France, Germany and Ireland, just to name a few. But first I want to reflect on some of the things I learned from this adventure.
My first takeaway is that I think there has to be more people living with cystic fibrosis than we think there are. Currently, the general accepted number is about 75,000 people living with CF on the planet at any one time. I think that is far too low. One thing I kept hearing is something to the effect of, “my [insert country] doesn’t have a complete cystic fibrosis registry. We know there are more people out there with CF, we just do not have the resources to diagnose them.” That specifically came up in the Russia interview, where my contact said it is theorized that there are about 10 times the number of registered/diagnosed patients living throughout the country.

By Indian Flag [CC BY-SA 4.0 (http://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons
It is very different for a child to seemingly die from pneumonia than it is for that same child to be diagnosed and treated properly for cystic fibrosis. People who may not be correctly diagnosed with cystic fibrosis in developing countries undoubtedly have little chance to survive.
I don’t claim to be someone who studies overall population trends or patterns, but if any of this proves to be true, I would place the total number of people living with cystic fibrosis across the globe to be over 200,000, rather than the ~75,000 we know of.
My second takeaway from the project so far is that the standard of care around the world is not where it should be. My heart goes out to the people living with cystic fibrosis in Macedonia, Russia and South Africa – to name a few places. It would be an understatement to say that I am concerned for the disease outcomes in those countries. I will say, however, that I am amazed with the resourcefulness of the CF families/patients in those parts of the world. Between the family in Russia buying a Vest out of pocket, the Macedonian family needing to bring medication in from other EU countries and the South African adult patient putting together the raw materials of medications for her own well being, it’s all simply amazing, and also frustrating at the same time. The medical infrastructure in those countries is failing these people – specifically in Macedonia where “there is a CF Association trying to lobby [the legal institutions] for [the patients] and their right to live. Yet there are a lot of obstacles to be overcome,” and South Africa where my contact avoids going to the hospital out of the fear of cross infection due to the lack of safety guidelines.
Ultimately what is most concerning is that it seems real help is not right around the corner. I hope that the awareness we are bringing to the patients living in these countries pays dividends to their standard of care quality of life as a patient – I recommend taking a look at Cystic Fibrosis Worldwide and supporting their initiatives.
The bottom line is that the access to medications and proper medical infrastructure for people with CF is critical to survival and disease management. As it stands there are people living with cystic fibrosis that do not have access to the standard of care that we enjoy in the United States – even as close as US Territories, like the Virgin Islands where we learned the CF family there has to travel to the states every few months for a clinic visit. Life with cystic fibrosis can be brutal and unforgiving, but if anyone is going above and beyond with CF, it is the people living in countries with developing medical outcomes.
I hope to learn more about people living with CF in the developing world.
Finally we have the contrast between the types of healthcare in developed nations. Ultimately healthcare is a little more complex than getting sick, going to the doctor, getting a prescription and then going to the pharmacy to pick up a medication. Healthcare is a delicate relationship between patients, care providers, medical institutions, drug developers (innovation of new medications), reimbursement agencies (insurance) and the government.
If anything, this project highlighted the vast differences all over the world as it relates to healthcare, or more simply put, a national health provider (Canada, Australia, Israel, UK, Spain, Denmark, and the Netherlands) vs. the American healthcare system. I’ve come to the conclusion that there has to be a middle ground, and here’s why: The Vest.
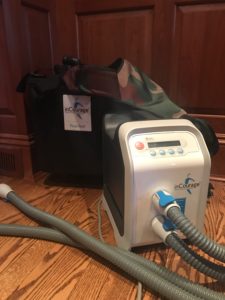
The United States CF population seems to be the only group that relies heavily on the Vest, whereas it is all but unavailable to people in other countries (with the few obvious exceptions – like people who buy a device out of pocket or receive one on compassionate grounds). The Vest is a costly machine, yet in the US it is not uncommon for CF families to own, or have owned, multiple Vest machines thanks to upgrades, difference models, out growing an older one or a number of different reasons. To that end Vest therapy is pretty much considered a typical CF treatment suitable for just about any CF patient dealing with respiratory issues.
Coming from my personal opinion (if you’re familiar with the CF community or in it yourself, you know every patient has a strong opinion about airway clearance), I’m not sure there is a clear rival to the Vest. I abandoned other methods of airway clearance a long time ago (except for the occasional day here or there) after noticing their lack of effectiveness compared to the Vest.
Abroad, people with CF rely on other methods of airway clearance (of which there are many), including manual chest PT, which is something Americans generally prefer only when hospitalized. To my knowledge there is no study that supports the Vest airway clearance system over other methods (of which there are several, i.e. the Areobika, Flutter, Accapella, CPT, etc.), so I think it would be interesting to study that, but I couldn’t help but ask myself, why is the Vest used so much in the US, compared to almost never around the world?
I suspect it is because of the price tag and the reluctance of national healthcare systems to foot such a large bill for a device that seemingly has no benefit over another method. The same seems to be true for next generation cutting edge medications as well. In Australia, specifically, where it seems like the CF community gets all the help they need from CF associations (which by the way is a fantastic system – take note, CFF), the patient population is fighting for government reimbursement of “corrector” medications.
There was a similar situation in Canada where my interviewee, Amanda, received a medication in a study and saw her lung function jump up 12%. After the study when she discontinued the medication she had to wait several years before she could receive the medication through a compassionate use program prior to the drug being approved by Health Canada. The medication has since been approved.
I think those examples alone underscore major issues amongst national healthcare initiatives, and we’re only talking about CF here. The governments that refuse to pay for the Vest and some of the newer medications are letting down their taxpaying cystic fibrosis patients and families. Should the United States follow in suit to that kind of nationalized healthcare system, I would be left feeling concerned that I would lose access to therapies we currently have, and any future ones that may seem pricey in the eyes of the government. If choices for patients abroad are being taken away, what’s to say that wouldn’t happen here under similar circumstances?
The way our healthcare system works in our country also undoubtedly correlates to medical innovation as seen through some of these interviews. I don’t think it’s a coincidence that major drug development is happening in the United States, rather than elsewhere in the world. Beyond that, and continuing to use the Vest as an example, nationalized healthcare system, as witness abroad, surely must seek to control drug prices. It makes sense. Governments will always try to conserve taxpayer dollars to control their respective budgets. Now, while that may seem fine and great on the surface, controlling prices serves no one in the long term and can have major consequences as far as drug development goes. Revenue fuels investment, and investment fuels innovation.
Now, with that being said, healthcare as it currently stands in this country can leave people feeling hesitant or scared, and I totally understand that, as there is still quite a bit to be desired with the old law that is crumbling and the new one that is passing through congress that no one seems to know much about.
As Jillian said in her USA interview, “I approach an age [26] where I have to take full financially responsibility for my CF, I struggle with the fears of what if I can’t afford [healthcare].” Jillian is not alone here. I hold the same reservations as I just turned 26. Compare this to the way William feels in the UK, “The National Health Service has provided me with free care and treatment all my life and free medication up to the age of 18. From 18 onwards I’ve paid for meds through a pre-payment of around £130 ($160) [and taxes].”
The difference here cannot be understated.
William has the security of feeling like he will always be covered at low cost regardless of his health. Here in the US, people don’t always feel that way, and that can be concerning because there will come a time in the lives of many people with CF, where we may not be able to provide for ourselves and become completely reliant on others and the care we are offered.
In the end it is clear that people living with cystic fibrosis, regardless of nationality, creed, financial stability or skin color are innocent victims. The same is true for people living with any genetic disability, whether it is sickle cell, Down syndrome, hemophilia or any of the others. We never had a choice in the life we were given, and as result we cannot be punished financially, or in any other way, for needing healthcare.
As a taxpayer, I expect my government to guarantee my care and supplement the cost of my care that is critical to sustain life – I am going to have to pay for my care, but I expect the government’s help. Without the proper choice of medications, people with CF have very little hope. We must be given that opportunity, whether or not we can provide for ourselves.
At the same time, however, I would not want to be in a position to need to lobby my government, based on cost alone, for access to medications that are proven to be effective. The United States can do better in the healthcare sector, but it is not something that I believe should be nationalized entirely, nor do I think it should be reformed in a way that compromises drug development and innovation.
We have to ask ourselves, do we want to continue along at the current pace with no new treatment options, or would we have access to the future of cystic fibrosis care? As the new healthcare law currently stands, I think it affords us the chance to have access to new medications and continued development of new medications, but ultimately it must guarantee access to the people who may not be able to afford it. With the way our congress works, the law will continue to change, so we must continue to advocate for all people living with CF.
Our national healthcare system should be there to help people who cannot provide for themselves, and the people with genetic pre-disposition to illness, like all of us living with CF. For example, I really cannot justify my tax dollars going to supplement care for someone who spent 30 years of his life smoking cigarettes without ever attempting to quit, only to find himself suffering from a smoking related illness. I can, however, justify my tax dollars going to help a little boy suffering from sickle cell.
I look to the BCMH program in Ohio as a way forward for people in the United States. Essentially it is a state funded program that covers the remaining cost left over from private insurers or Medicaid for those who are financially eligible. It’s a good example of the happy medium that I think people with genetic illness must absolutely be afforded.
This ended up being way longer than I sort of hoped it would be, but I think it goes without saying that people with cystic fibrosis around the world must absolutely be given a chance to succeed. We are seeing that happen in some places, while patient populations are being overlooked in others. My aim with this project has been to talk directly with patients and their families, rather than seeking some third-party study. People will forever be their own best advocates.
I hope that cystic fibrosis will be looked at as a global issue – a community of patients in need of help from everywhere until we can all breathe easy. Until then, this program, Cystic Fibrosis Around the World, will be a work in progress.
*Cystic Fibrosis Research Inc. (CFRI) Newsletter, Summer 2013